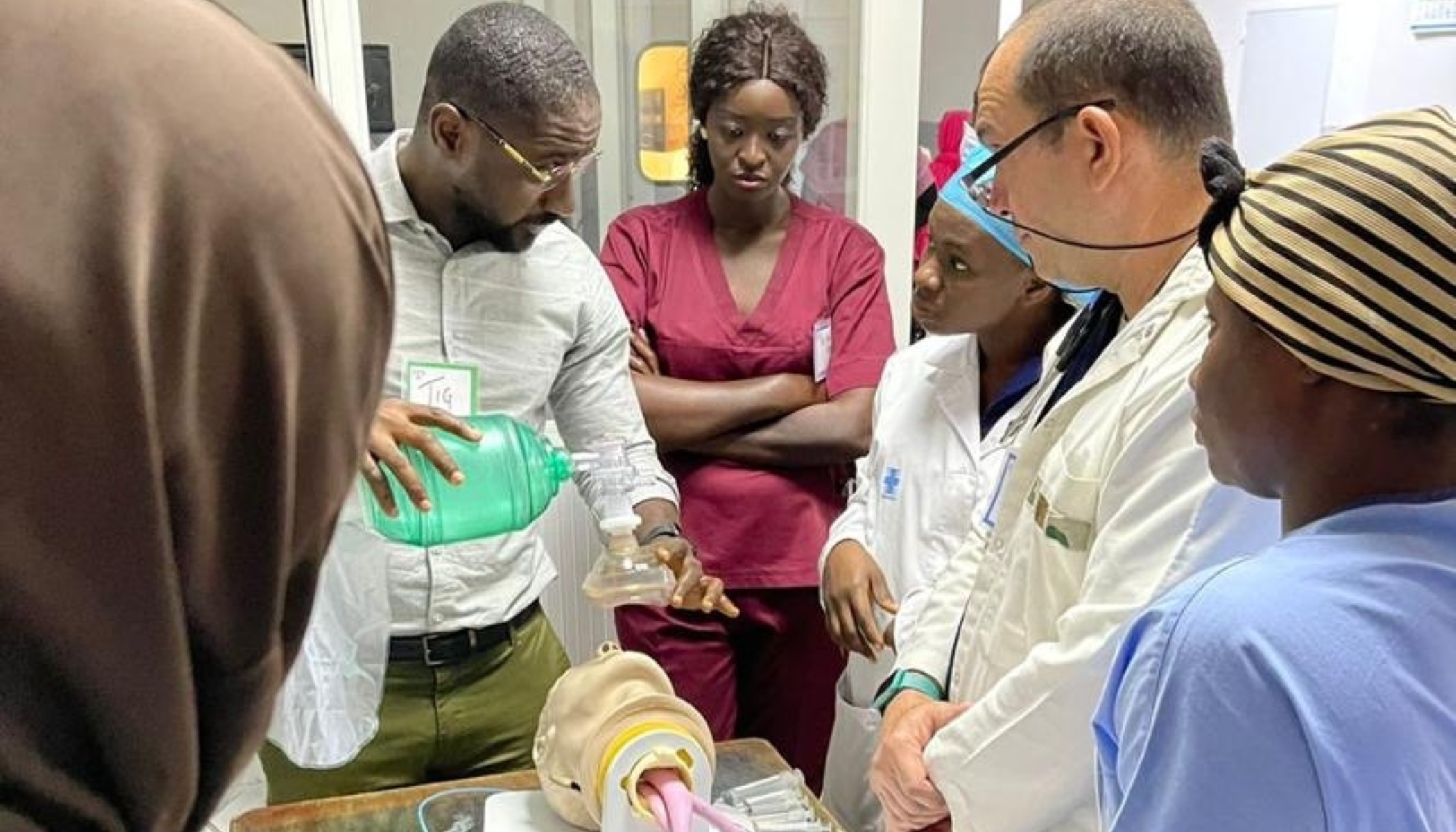
Dr. Maimie shares his experiences as one of the first participants of the innovative Liberia Anaesthesia Capacity Building Programme, which supports Liberian physicians to become the country’s first homegrown anaesthesiologists.
By Dr Kpehe Jig Maimie
With a population of almost 5 million, Liberia has never had a physician anaesthetist of Liberian origin working in the country, with the responsibility for anaesthesia provision falling instead on around 70 anaesthetic nurses.
Created to help boost the anaesthesia workforce, the Liberia Anaesthesia Capacity Building Programme (LACBP) trains Liberian-born doctors, such as myself, to undertake the West Africa College of Surgeons (WACS) diploma in anaesthesia at Aminu Kano Teaching Hospital (AKTH), Nigeria. I was selected in 2018 as one of the first four physicians to participate, and I successfully received my WACS diploma in 2020.
WACS-certified physicians can then continue on the LACB programme and train toward becoming fully-fledged anaesthesiologists. Now a senior resident, and having passed my Membership exams, I have continued to work at AKTH towards the WACS Fellowship exam, the final certification of the extended programme.

A working week as a resident
To graduate from the extended programme, candidates must log over 1000 surgical cases across diverse specialities and sit a week of exams that include written papers, a long case, oral exams, and OSCE.
A workday for a senior registrar at the hospital commences a day in advance by reviewing the scheduled surgical patients tailoring anaesthetic plans for them and then updating the covering consultant.
Each weekday morning, we start with ICU rounds, bedside patient care discussions and exam-focused skills. The residents then move to the operating theatres to attend to our surgical lists. Although the workday typically ends at 5 p.m., it may extend up to 11 p.m. for extensive and complex surgical cases.
Friday is reserved for academic activities. There are scheduled didactic lectures, resident presentations, departmental morbidity and mortality reports, and journal club reviews.
A huge source of joy for me is volunteer work, which I do in my spare time. I’ve served as a facilitator for the Safer Anaesthesia From Education (SAFE) Obstetrics course and the Mercy Ship’s Neonatal Resuscitation Programme in both Liberia and Gambia. These courses are designed to upgrade the skills and knowledge of physician anaesthetists, obstetricians, nurses and midwives.


Training in the OR
As an accredited tertiary centre, AKTH has superior perioperative capabilities and staffing in comparison to hospitals in Liberia.
During my training, I’ve participated in numerous renal transplant procedures successfully. I’ve also taken part in many pioneering procedures for the first time, including Cochlear transplant surgery and – more recently – open heart surgeries.
To say the least, embarking on this path has been exciting, from advocating patient safety and satisfaction to administering drugs with seemingly magic effects daily, as well as using the amazing gadgets in the OR.
Of the many cases I have handled in the OR, the case of a 16 girl scheduled for an emergency appendectomy had a particularly profound impact on me. It was a key learning experience, teaching me that although we offer every case our all, there will be some days when even your best effort will never be good enough:
| Case Study | |
| Case Details | The patient, a 16-year-old female with sickle cell disease (Hbss), had a history of osteomyelitis and had been immobile for 7 months, was scheduled for an emergency appendectomy. She was reviewed preoperatively and appeared pale, in considerable pain, with moderate tachycardia and tachypnoea. Her steady-state Hb level was 8.5g/dl, while other laboratory findings were within normal reference ranges. Her ASA status assigned was III E. |
| Surgery | Supplemental oxygen and fluid therapy was initiated before the surgery, and the patient chose General Anesthesia. Two units of blood were secured, and she was taken to the operating room. Although the case was straightforward, a senior registrar was present when anaesthesia was administered. She received preoxygenation, underwent rapid sequence induction, and was intubated. Adequate analgesia, hydration, oxygenation and normothermia were maintained throughout the surgery. The surgery lasted 30 minutes with a minimal blood loss of 100 ml. |
| Post-surgery | Post-surgery, she was extubated awake with intact airway reflexes. However, as she was transferred to the recovery area, she suffered rapid desaturation with hypotension. Despite administering oxygen and fluid resuscitation, her saturation failed to improve. Re-intubation was performed, but saturation still did not recover, leading to cardiac arrest. The unit consultant was informed, and CPR was initiated, yet efforts were unsuccessful. She passed away with Massive Pulmonary Embolus as the likely cause of death. Palpable sadness hit the entire team. Even after three years, I still vividly recall her memory. |
Challenges
Life as a resident at AKTH can definitely be challenging, and its many demands require significant resilience, focus and determination, but the overall experience has proved equally rewarding. To combat challenges, I pray, meditate, exercise and travel as often as I can – I’ve found all of these helpful wellbeing and resilience strategies.

It’s common to experience a heavy sense of nostalgia, particularly when separated from wives and children, though their support has been unwavering. My journey has also been marked by difficult moments, including the loss of some of my closest colleagues, mentors and father figures, including Dr Keith Thompson, a creator of the LACB programme, whose invaluable lessons will be forever cherished.
The staff at AKTH, including the Chief Medical Director (CMD) and Anaesthesia Department (our extended family), have offered gracious support. Following our success in achieving the WACS Diploma, the current CMD of AKTH, Prof. Abdurrahman A. Sheshe, hosted us for a befitting lunch!
Looking ahead
At home in Liberia, substantial efforts have been taken to enhance the perioperative capabilities of health facilities, and there has been a drive towards strengthening and building a resilient anaesthesia community.
I commend the Liberian government’s initiative in sponsoring anaesthetist training to help bolster the workforce. This marks a shift away from the reliance on nurse anaesthetists staffing all tiers of health facilities, though we remain grateful to our nurse anaesthetists for keeping the system moving.
But there is still more work to do. Ensuring the success of the anaesthesia workforce requires unity, and physician and nurse anaesthetists must continue to collaborate in prioritising patient care.
To aspiring African doctors – particularly those from Liberia who are yet to finalise their career choices – I ask you to consider anaesthesia as a prospective option. Together, with determination, focus and resilience, we can enhance access to safe anaesthesia and surgery in Liberia.
About the LACBP
Developed by Dr. Keith Thomson and Prof. Alhassan Datti Mohammed, the LACBP was launched in 2018 as a collaboration between the World Federation of the Societies of Anaesthesiologists (WFSA), the Liberian Medical & Dental Association (LMDA) and the Nigerian Society of Anaesthetists (NSA). This programme has been made possible by generous contributions from Diamedica, the Association of Anaesthetists, the Shalimar Trust and Dr Keith Thomson.